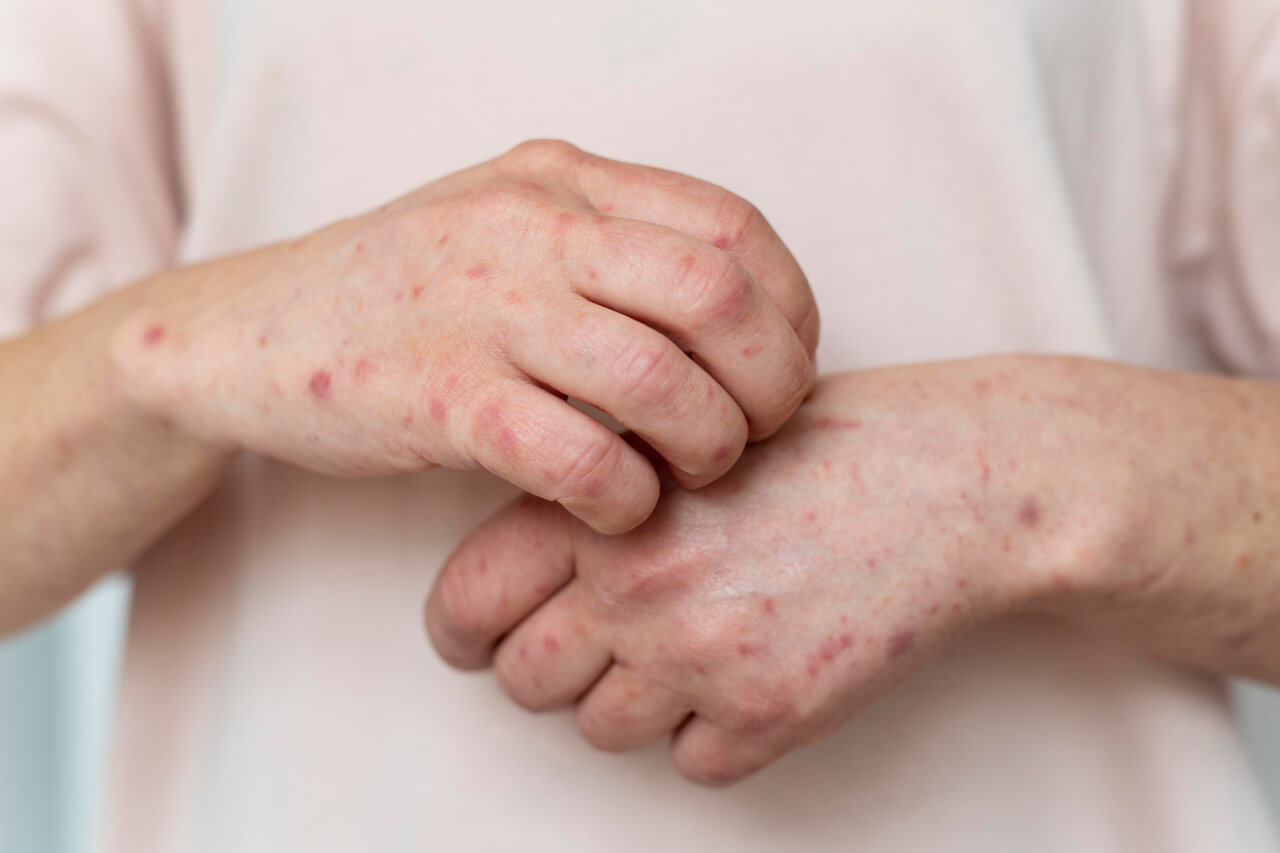
Contact dermatitis is a skin condition characterized by inflammation of the skin that occurs when it comes into contact with certain substances.
This condition is not contagious or life-threatening, but it can cause discomfort and distressing symptoms.
Types of Contact Dermatitis
It can be classified into two main types based on the mechanism of skin reaction: irritant contact dermatitis (ICD) and allergic contact dermatitis (ACD).
Irritant Contact Dermatitis (ICD)
This is the more common type and is caused by direct damage to the skin by a substance.
Irritants may include chemicals, soaps, detergents, solvents, acids, or other substances that strip away the skin’s natural oils and disrupt its protective barrier.
Common examples include prolonged exposure to water, certain cleaning products, or harsh chemicals.
Allergic Contact Dermatitis (ACD)
This type occurs when the immune system reacts to a substance as if it were harmful, even though it may not be.
The body’s immune response leads to an inflammatory reaction in the skin.
Common allergens include certain metals (such as nickel), latex, certain plants (like poison ivy or poison oak), and certain cosmetics or personal care products.
Symptoms
Contact dermatitis can manifest with a variety of symptoms, and the specific signs can vary depending on the type of contact dermatitis (irritant or allergic) and individual factors.
Here are common symptoms associated with contact dermatitis:
Redness (Erythema)
One prominent symptom is redness, clinically referred to as erythema.
This discoloration occurs due to increased blood flow to the affected area as a result of the inflammatory response triggered by exposure to an irritant or allergen.
Itching (Pruritus)
Itching, or pruritus, is another common and often bothersome symptom associated with the condition.
The itching sensation is a consequence of the inflammatory processes and the irritation of nerve endings in the skin.
This symptom can range from mild to severe, leading individuals to scratch the affected area, potentially exacerbating the condition.
Swelling (Edema)
Swelling, or edema, is frequently observed in contact dermatitis.
The inflammatory response can cause fluid to accumulate in the tissues, resulting in a swollen and sometimes puffy appearance.
In more severe cases, blisters, or vesicles, may form. These fluid-filled sacs develop as a result of the body’s attempt to protect and repair the skin, isolating it from the irritant or allergen.
Rash
The development of a rash is a hallmark symptom of contact dermatitis.
The rash typically appears as red, inflamed patches on the skin and can vary in size and shape.
The skin may also become dry, rough, or cracked, indicating a disruption of the skin barrier.
Dry or cracked skin is often more prominent in irritant contact dermatitis, where direct damage to the skin occurs.
Burning or Stinging Sensation
Burning or stinging sensations are reported by individuals with the condition.
These sensations are a result of nerve irritation and heightened sensitivity in the affected area.
Pain or discomfort may also accompany contact dermatitis, especially if blisters or open sores develop.
The inflammatory response and irritation of nerve endings contribute to these sensations.
Oozing or Weeping
In severe cases, oozing or weeping of fluid from the affected skin may occur.
This is a sign of significant inflammation and the body’s attempt to repair the damaged skin.
Scaling or peeling of the skin can be observed as the affected area undergoes regeneration following the resolution of inflammation.
Recognizing these symptoms is crucial for identifying and managing contact dermatitis effectively.
Causes
Contact dermatitis can be caused by exposure to irritating substances or allergens, leading to inflammation of the skin.
Irritant Contact Dermatitis (ICD)
Irritant contact dermatitis is a common form of skin inflammation caused by direct exposure to substances that physically or chemically damage the skin.
Harsh chemicals and solvents found in cleaning products, industrial settings, or certain occupational environments are common culprits.
Prolonged or frequent contact with soaps and detergents can strip the skin of its natural oils, leading to irritation.
Water, especially in activities like dishwashing or frequent handwashing, can also contribute to ICD by weakening the skin barrier.
Essentially, any substance that can cause direct harm to the skin, either through its abrasive nature or by disrupting the skin’s protective layers, has the potential to induce irritant contact dermatitis.
Allergic Contact Dermatitis (ACD)
Allergic contact dermatitis is an immune-mediated response triggered by exposure to a specific substance, or allergen, to which an individual has become sensitized.
This means that the person has been previously exposed to the allergen, and their immune system has developed an exaggerated response to it.
Common allergens include metals like nickel, which is frequently found in jewelry, and fragrances present in many cosmetics and personal care products.
Preservatives, such as parabens, in skincare items can also be allergenic.
Plants like poison ivy contain urushiol, an irritant that can induce ACD upon contact.
Additionally, latex found in gloves and medical devices can cause allergic reactions in sensitive individuals.
Unlike irritant contact dermatitis, ACD involves the immune system mounting an inflammatory response to the perceived threat, leading to characteristic symptoms.
Photocontact Dermatitis
Photocontact dermatitis is a unique form of contact dermatitis where a substance applied to the skin becomes allergenic when exposed to sunlight (UV radiation).
In these cases, the combination of the substance and UV light triggers an immune response, leading to skin inflammation.
This type of contact dermatitis underscores the importance of considering environmental factors, such as sunlight exposure, in understanding and managing skin reactions.
Identifying the specific cause of contact dermatitis is crucial for effective management.
Diagnosis
The diagnosis of contact dermatitis involves a thorough evaluation by a healthcare professional, typically a dermatologist.
The process includes gathering a detailed medical history, conducting a physical examination, and, in some cases, performing specific tests to identify the causative agents.
Here is a detailed explanation of the steps involved in diagnosing contact dermatitis:
Medical History
The healthcare provider will begin by taking a comprehensive medical history.
They will inquire about the patient’s symptoms, the duration and pattern of the rash, any known triggers or exposures, and the patient’s occupation and hobbies.
Information about the use of skincare products, cosmetics, and potential allergens in the environment will be gathered.
A detailed occupational history is important, especially for identifying potential irritants or allergens in the workplace.
Physical Examination
A thorough physical examination of the affected skin is conducted.
The healthcare provider will examine the distribution, appearance, and characteristics of the rash.
They may also assess the severity of symptoms, including redness, swelling, itching, and the presence of blisters.
The examination may include an evaluation of other areas of the skin to check for the presence of similar or related rashes.
Patch Testing (for Allergic Contact Dermatitis – ACD)
Patch testing is a specialized diagnostic test used to identify specific allergens that may be causing allergic contact dermatitis (ACD). It is typically performed by a dermatologist.
During patch testing, small amounts of common allergens are applied to patches, which are then placed on the patient’s back.
The patches remain in place for a specific period (usually 48 hours) before being removed.
After the patches are removed, the dermatologist evaluates the skin for any signs of allergic reactions, such as redness and inflammation.
This helps identify specific allergens to which the patient may be hypersensitive.
Phototesting (for Photocontact Dermatitis)
If photocontact dermatitis is suspected, phototesting may be performed.
This involves exposing the skin to ultraviolet (UV) light after applying potential photosensitizing substances.
The goal is to observe if a reaction occurs due to the combination of the substance and UV light.
Blood Tests (rarely)
In some cases, blood tests may be conducted to assess the immune response and rule out other potential causes of skin inflammation.
However, blood tests are not commonly used for routine diagnosis of contact dermatitis.
Once the healthcare provider has gathered all relevant information from the medical history, physical examination, and any diagnostic tests, they can make a definitive diagnosis of the type of contact dermatitis and identify specific triggers or allergens.
5 Effective treatments
The treatment of contact dermatitis involves a combination of strategies to alleviate symptoms, promote healing, and prevent further exposure to irritants or allergens.
Here are five effective treatments for contact dermatitis:
Avoidance of Triggers
The most critical aspect of managing contact dermatitis is identifying and avoiding the substances that trigger the condition.
Once the irritant or allergen is identified through methods like patch testing, the patient is advised to minimize or eliminate exposure.
This may involve changes in personal care products, skincare routines, or occupational practices to prevent contact with known triggers.
Individuals with allergic contact dermatitis (ACD) may need to carefully read product labels to identify and avoid specific allergens.
In occupational settings, implementing protective measures such as wearing gloves can help prevent exposure to irritants.
Topical Corticosteroids
Topical corticosteroids are commonly prescribed to reduce inflammation and relieve symptoms such as redness, itching, and swelling.
These medications work by suppressing the immune response and reducing the activity of inflammatory substances in the skin.
Corticosteroids come in various strengths, and the choice of strength depends on the severity of the symptoms and the location of the affected skin.
Lower-strength formulations are typically used on the face and other sensitive areas, while higher-strength formulations may be used on thicker skin.
Topical Calcineurin Inhibitors
Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, are another class of medications used to treat contact dermatitis.
They modulate the immune response in the skin and are particularly useful in sensitive areas, like the face and neck.
These medications are often considered for individuals who may be sensitive to or cannot use topical corticosteroids.
They are generally prescribed for short-term use and may be part of a maintenance plan to prevent flare-ups.
Emollients and Moisturizers
Emollients and moisturizers play a crucial role in managing contact dermatitis by helping to repair the skin barrier and prevent dryness.
Regular use can reduce the risk of flare-ups and alleviate symptoms.
Choose fragrance-free and hypoallergenic products to minimize the risk of irritation.
Emollients with ingredients like ceramides, fatty acids, and glycerin can be particularly effective in maintaining skin hydration.
Oral Antihistamines
Oral antihistamines, such as cetirizine, loratadine, or diphenhydramine, can be used to relieve itching and improve sleep quality, especially if symptoms are disrupting normal daily activities or causing discomfort.
Antihistamines are more commonly used in cases where itching is a predominant symptom.
They do not directly address the underlying inflammation but can provide symptomatic relief.
It’s important to note that the choice of treatment depends on the type and severity of contact dermatitis, as well as individual factors.
Preventions Tips
Preventing contact dermatitis involves minimizing exposure to irritants and allergens, maintaining a healthy skin barrier, and adopting practices that reduce the risk of skin reactions.
Here are tips to help prevent contact dermatitis:
Identify and Avoid Triggers
The first step in prevention is identifying substances that trigger contact dermatitis.
If you have a known sensitivity or have experienced skin reactions, read product labels carefully to identify potential irritants or allergens.
Consider patch testing if the specific triggers are unclear.
Be aware of common allergens like nickel in jewelry, fragrances in cosmetics, and certain preservatives in skincare products.
In occupational settings, follow safety guidelines and use protective equipment to minimize exposure to irritants.
Choose Hypoallergenic Products
Opt for skincare products, cosmetics, and detergents labeled as “hypoallergenic” or “fragrance-free.” These products are formulated to be less likely to cause allergic reactions or irritation.
Check ingredient lists for potential allergens or irritants.
Avoid products with a long list of chemicals or those containing known allergens if you have sensitive skin.
Use Protective Measures
In situations where contact with irritants is inevitable, use protective measures such as gloves and other personal protective equipment.
This is particularly important in occupational settings where exposure to chemicals or irritants is common.
Choose gloves made of materials that provide a barrier against specific substances.
Ensure that gloves are clean and in good condition. In some cases, double gloving may provide extra protection.
Practice Good Hand Hygiene
Frequent handwashing is essential for hygiene but can contribute to irritant contact dermatitis.
Use a mild, fragrance-free soap and lukewarm water. Moisturize hands immediately after washing to prevent dryness.
Consider using hand sanitizers with moisturizing agents if handwashing is not possible.
Choose moisturizers containing ingredients like ceramides and glycerin for effective hydration.
Moisturize Regularly
Keeping the skin well-hydrated is crucial in preventing contact dermatitis.
Moisturizers help maintain the skin barrier, reducing the risk of irritation and promoting overall skin health.
Use emollients or moisturizers regularly, especially after bathing or handwashing.
Choose products without fragrances, dyes, or other potential irritants.
Apply moisturizer to damp skin for better absorption.
Be Cautious with Jewelry
Certain metals, particularly nickel, can cause allergic reactions in susceptible individuals.
Choose jewelry made of hypoallergenic materials such as stainless steel, titanium, or nickel-free alloys.
If you have a known nickel allergy, avoid wearing nickel-containing jewelry.
Consider applying clear nail polish to create a barrier between the metal and your skin.
Sun Protection for Photocontact Dermatitis
If you are prone to photocontact dermatitis, use sun protection measures.
This includes applying broad-spectrum sunscreen with high SPF to exposed skin and wearing protective clothing.
Choose sunscreens labeled as suitable for sensitive skin and free from common irritants or allergens.
Reapply sunscreen as directed, especially after swimming or sweating.
Be Mindful of Occupational Exposures
In occupational settings, be aware of potential exposures to irritants or allergens.
Follow safety guidelines, use protective equipment, and seek alternatives, if possible, to minimize contact with substances that can trigger dermatitis.
Consult with occupational health professionals to assess workplace risks and identify preventive measures.
Implementing engineering controls and proper ventilation can also reduce the risk of exposure.
By incorporating these preventive measures into your daily routine and being mindful of potential triggers, you can significantly reduce the risk of developing contact dermatitis.
If you have a history of skin reactions or suspect contact dermatitis, seek guidance from a healthcare professional or dermatologist for personalized advice and recommendations.
Conclusion
Contact dermatitis is a common skin condition characterized by inflammation resulting from exposure to irritants or allergens.
The two primary types, irritant contact dermatitis (ICD) and allergic contact dermatitis (ACD), have distinct causes and mechanisms.
Diagnosing contact dermatitis requires a thorough evaluation by a healthcare professional, involving a detailed medical history, physical examination, and, in the case of ACD, patch testing.
Once diagnosed, effective treatment strategies can be implemented. These may include avoidance of triggers through lifestyle and occupational adjustments, the use of topical corticosteroids or calcineurin inhibitors to manage inflammation, and the incorporation of emollients and moisturizers to maintain skin hydration.
Preventing contact dermatitis involves proactive measures such as identifying and avoiding triggers, choosing hypoallergenic products, using protective measures in occupational settings, practicing good hand hygiene, and moisturizing regularly.
Additionally, being cautious with jewelry, employing sun protection for photocontact dermatitis, and being mindful of occupational exposures can contribute to a comprehensive prevention strategy.
Understanding the causes, symptoms, diagnosis, and effective treatments for contact dermatitis empowers individuals to take control of their skin health.
In cases of persistent or severe symptoms, seeking guidance from a healthcare professional, particularly a dermatologist, is crucial for accurate diagnosis and personalized management plans.
By adopting preventive measures and appropriate treatments, individuals can manage and reduce the impact of contact dermatitis on their quality of life.
FAQs
What is contact dermatitis?
Contact dermatitis is a skin condition characterized by inflammation resulting from exposure to irritants or allergens.
What are the common symptoms of contact dermatitis?
Symptoms include redness, itching, swelling, rash, and, in severe cases, the development of blisters.
What are the main types of contact dermatitis?
The main types are irritant contact dermatitis (ICD), caused by direct damage to the skin, and allergic contact dermatitis (ACD), an immune-mediated response to specific allergens.
What are effective treatments for contact dermatitis?
Treatments include avoiding triggers, using topical corticosteroids or calcineurin inhibitors, employing emollients, and, in some cases, oral antihistamines.
How can contact dermatitis be prevented?
Prevention involves identifying and avoiding triggers, choosing hypoallergenic products, using protective measures, practicing good hand hygiene, and moisturizing regularly.